Access to Medicines: What Happens if a COVID-19 Vaccine is Discovered?
archive


(Photo credit: Xinhua/Zhang Yuwei via Getty Images)
Access to Medicines: What Happens if a COVID-19 Vaccine is Discovered?
Presently, there is an urgent and concerted worldwide effort to discover a vaccine for COVID-19, with about 150 drugs being researched.1 But what happens if one or more effective vaccines are discovered? More particularly, what kinds of legal barriers arise for countries seeking to manufacture or import the vaccine to immunize their people?
If an effective vaccine is discovered in a university or some other institution, it will patent the medicine, but it may lack the capacity to manufacture and distribute the vaccine on a large scale. It is therefore likely assign the rights to a large pharmaceutical company (Big Pharma) in return for royalty payments or a one-off payment. Big Pharma will then effectively receive most if not all the monopoly rights of the patent-holder.
Monopoly patent rights are precious, particularly as they allow monopoly pricing. This can place access to medicines out of reach for all except those with deep enough pockets, or to those to whom Big Pharma chooses to provide access at lower prices.
Most countries are members of the World Trade Organization (WTO). Member countries are bound by the terms of the agreement on Trade Related Aspects of Intellectual Property Rights (TRIPS). A country that enacts laws inconsistent with their TRIPS obligations can be subjected to the WTO disputes settlements process and possibly punished for violations. TRIPS obligations include that each member country’s laws provide at least 20 years patent protection for inventions (including inventions of new medicines).
Yet Articles 31 and 31bis of TRIPS also allow governments to pass laws for compulsory licensing of an invention. This could allow for the manufacture and distribution of a specified medicine in a country, despite any lack of permission (i.e. a license) from the patent-holder. But TRIPS only allows a government to compulsorily license an invention (including a vaccine) if it believes a patent holder is ‘abusing’ its patent rights, including in circumstances where it undermines the protection of public health.2 So, restricting the distribution of a patented antiviral or imposing excessive prices could be seen to be an abuse of the patent. Compulsory licensing generally allows a government to manufacture and distribute (and in the case of least-developed countries, import) the drug at a much cheaper price and ensure widescale distribution and administration of the drug.
Lawmakers in a number of countries including Chile,3 Israel,4 Ecuador,5 Canada,6 and Germany7 have already enacted laws or adopted resolutions for the compulsory licensing of COVID-related drugs or vaccines. On the face of it, this seems reassuring, but hurdles to providing access to medicines have been erected over the years with the connivance of Big Pharma. One of the most effective strategies involves the adoption of bilateral and multilateral trade treaties that include "TRIPS-plus" provisions concerning intellectual property rights. For instance, Article 12 requires that national laws set a minimum of 50 years copyright protection. However, a country can go beyond the minimum and set, say, a 70-year period of copyright protection.
A substantial number of multilateral and bilateral trade agreements include TRIPS-plus provisions that extend the rights of Big Pharma over their patented drugs. These can delay the capacity of manufacturers to produce generic (and substantially cheaper) versions of a drug well beyond a Big Pharma’s 20-year patent period.8
The TRIPS-plus provisions typically extend Big Pharma rights by requiring countries that are parties to a bilateral or multilateral trade agreement to enact laws that include granting patents for "new uses of known products, new methods of using known products, or new processes of using known products" and adjusting patent terms "to compensate for delays in granting patents and/or in marketing approval processes."9 The TRIPS-plus provisions can also include "data protection" requirements. The data might include information about clinical trials, which a generic manufacture would need to market the medicine.
TRIPS only allows a government to compulsorily license an invention (including a vaccine) if it believes a patent holder is ‘abusing’ its patent rights...
In my view, the TRIPS-plus provisions are inconsistent with Article 8 of the TRIPS Agreement to the extent they purport to limit a country’s power to enact laws “necessary to protect public health and nutrition, and to promote the public interest in sectors of vital importance to their socio-economic and technological development,” if those laws are consistent with the other provisions of TRIPS. In other words, Article 8 can be understood as preserving the rights of WTO members to enact laws to protect public health, and any bilateral or multilateral agreement that purports to limit the power of lawmakers to make those laws is inconsistent with TRIPS.
In all likelihood, Big Pharma will play the long game. It cannot risk serious reputational damage by inhibiting access to a COVID-19 vaccine during the pandemic. Indeed, the current crisis offers an opportunity to show what good global citizens Big Pharma are, giving them sufficient reputational credits with lawmakers to push for further advances of monopoly powers in the future. As an indicator of the behavior we can expect from Big Pharma in the future:
Gilead Sciences looked like a good corporate citizen when it reported that one of its patented investigational drugs, remdesivir—an antiviral treatment mostly invented and researched by a consortium of NIH-funded academic labs—had potential as a COVID-19 cure.… [However, the] company quietly attempted to extend its monopoly on remdesivir and gain extra tax credits using a loophole that closes after 200,000 patients are infected by the disease targeted by the drug.10
Similarly, Big Pharma will seek to manage its monopoly rights for a COVID-19 vaccine on its own terms. This will probably involve rapid-fire licensing arrangements with generics manufacturers around the world, allowing for the manufacture and pervasive worldwide distribution of the vaccine. Under the cover of a pandemic, Big Pharma will dictate licensing terms, which will doubtless have a sting in their tail. The licenses may say that Big Pharma decides when the COVID-19 emergency is over, allowing it to take tighter control over post-crisis distribution and pricing.
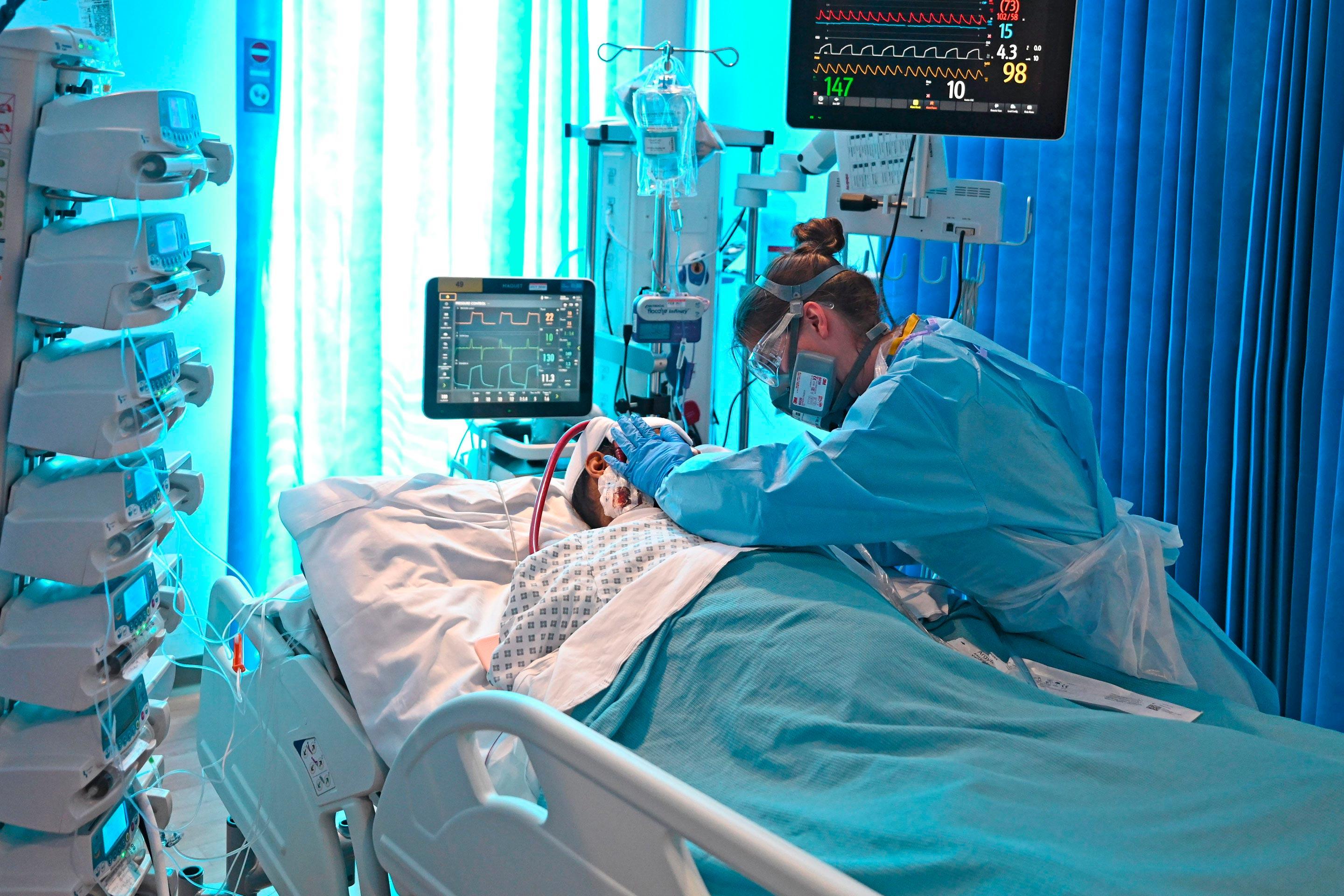
A Cambridge, England hospital participating in a U.K. drug trial for COVID-19. (Photo credit: Getty Images)
National governments nevertheless retain considerable authority to enable access to any new vaccine at affordable prices if they are willing to do so. The greatest risk is that national governments may step aside and allow Big Pharma to act bloodlessly in its own self-interest. As Zaitchik aptly observes: “The industry has produced staggeringly high margins by pushing prices to their breaking point on drugs developed through a $42 billion annual subsidy dispersed by the National Institutes of Health. That the same companies are now posturing before an anxious world as avatars of innovation and selflessness is the crowning irony of the coronavirus crisis.”11 This observation points to a larger problem: “As the world shifts its focus from containment to a cure, it’s become urgent to face up to the dangers of our reliance on pharmaceutical and biotech industries built to serve Wall Street and shareholder value over human needs and public health.”12
Without proper and effective government engagement, Big Pharma will leverage the pandemic to maintain the pretense that current arrangements are the best means for advancing drug development to benefit society. It will continue to claim it can serve society better if its monopoly rights could be extended even further. If Big Pharma succeeds with such claims, society will be left worse off than before the pandemic. National governments must, at the very least, maintain high levels of vigilance and take the initiative by retaining control of the manufacturing, distribution, and importing of any COVID-19 vaccine in the public interest.
Without proper and effective government engagement, Big Pharma will leverage the pandemic to maintain the pretense that current arrangements are the best means for advancing drug development to benefit society.
Although compulsory licensing during a national emergency will provide a short-term response to heading off rapacious pricing and limited access to an antiviral, it will not address the broader structural problems that exist with our present system. Major structural reforms are needed that extend well beyond existing initiatives, including the Drugs for Neglected Diseases initiative that operates in collaboration with the World Health Organization.13 Bold, committed and urgent reforms are required, potentially involving not only governments but also universities, donors, and (maybe) some industry members. This needs to be done not only in preparation for future virus pandemics but also to deal with increasing bacterial resistance to antibiotics,14 and the present woeful neglect in developing drugs for diseases prevalent in developing countries, including malaria.
If anything positive is to be gained from this pandemic, it is that it spurs a radical transformation of our systems for developing and providing access to medicines. If we fail to do so, the COVID-19 pandemic will be the bellwether for things to come.
1. J. Gallagher, “Coronavirus cure: When will we have a drug to treat it?” BBC News, 27 May 2020 https://www.bbc.com/news/health-52354520
2. J Malbon, C Lawson and M Davison, The WTO Agreement on Trade Related Aspects of Intellectual Property Rights: A Commentary (Edward Elgar, Cheltenham, UK, 2014) at 464.
3. https://www.keionline.org/chilean-COVID--resolution
4. https://www.law360.com/articles/1255079/israel-defies-abbvie-ip-to-import-generic-drugs-for-COVID--19
5. https://www.keionline.org/32429
6. COVID--19 Emergency Response Act, https://laws-lois.justice.gc.ca/eng/AnnualStatutes/2020_5/
7. https://www.whitecase.com/publications/alert/COVID--19-and-data-protection-compliance-germany
8. Gleeson, D., Lexchin, J., Labonté, R. et al. “Analyzing the impact of trade and investment agreements on pharmaceutical policy: provisions, pathways and potential impacts.” Global Health 15, 78 (2019). https://doi.org/10.1186/s12992-019-0518-2, p.4.
9. ibid., p. 6.
10. A Zaitchik, “No Antivirus in Sight.” The New Republic May 11, 2020.
11. ibid.
12. ibid.
13. https://www.dndi.org/achievements/gardp/
14. Simpkin, V., Renwick, M., Kelly, R. et al. “Incentivising innovation in antibiotic drug discovery and development: progress, challenges and next steps.” Journal of Antibiotics 70, 1087–1096 (2017). https://doi.org/10.1038/ja.2017.124



